Postoperative X-rays After Routine Orthopaedic Hardware Removal Following Lower Extremity Trauma: Are They Really Necessary?
Mergim Bajraliu, BcS, Kempland C. Walley, BcS, Eric Loesch, BcS, John Y. Kwon, MD
The authors report no conflict of interest related to this work.
©2016 by The Orthopaedic Journal at Harvard Medical School
BACKGROUND It is a commonly accepted practice for surgeons to obtain radiographs following removal of orthopaedic implants. Several studies have demonstrated the limited utility of routine post-operative imaging following various orthopaedic procedures. The purpose of this study was to evaluate orthopaedic patients who have undergone removal of hardware after lower extremity trauma to determine whether their expected post-operative course was altered based on the routine post-operative imaging they received.
METHODS Lower extremity removal of hardware procedures from 2008-2013 at a level 1 trauma center were reviewed. Patients undergoing removal due to pain attributable to the implanted hardware were eligible, whereas patients undergoing removal of hardware for any other reason were excluded. A total of 263 patients underwent removal of hardware; 103 patients met the inclusion criteria.
RESULTS Of the 103 eligible patients, post-operative radiographs did not alter the expected course for 103 (100%) patients. All patients in the cohort were followed for a minimum of 6 weeks post-operatively, and typically re-examined at 1 year from their index procedure.
CONCLUSION The routine utilization of post-operative imaging after removal of hardware did not change patient management and may be unnecessary. To reduce unnecessary costs and radiation exposure, radiographs should not be obtained following routine removal of orthopaedic implants.
Lower extremity trauma often necessitates the insertion of metallic implants (i.e.“hardware”) such as plates, screws, pins and rods for the reduction and stabilization of fractures. Removal of hardware is extremely common and accounts for as much as 33% of all planned orthopaedic procedures.1 Given the frequency of this procedure, it is imperative that best practices are instituted.
Radiography is vital to the effective treatment of orthopaedic patients. However, radiological images should offer some diagnostic or prognostic value. The routine post-surgical utilization of radiographs may not be warranted.
The rising cost of healthcare has placed the entire system under increased scrutiny. The use and costs of imaging services have increased twice the rate of all other health care technologies.2 Thus, the overuse of imaging is of particular concern.
Beyond cost, there is increasing concern regarding the exposure of patients to ionizing radiation. Medical imaging represents the largest source of ionizing radiation to the U.S. population.3 Although the effects of low levels remain relatively uncertain, researchers assert that the risk of cancer4 and cardiovascular disease5 are dose-dependent. Radiographs taken in the operating room expose both patients and hospital staff to radiation. Thus, it is imperative that imaging studies be conducted only when clinically indicated to limit exposure.
Furthermore, long office wait times continue to be a source of frustration for patients and their treating physicians. As a result, general patient satisfaction has been on a decline.6 Unwarranted imaging may contribute to this problem. In order to reduce wait times and increase patient satisfaction, it is imperative that all scheduled patients are receiving efficient care of the appropriate value.
Researchers have challenged the practice of ordering routine post-operative radiographs following various orthopaedic procedures including anterior lumbar interbody fusion,7 hip fracture fixation,8,9 hallux valgus correction,10 and total knee arthroplasty.11 However, the number of studies conducted on post-operative imaging of orthopaedic trauma patients is limited. To our knowledge, no studies have assessed the utility of post-operative radiography following routine removal of hardware. Given how commonly removal of hardware is performed, it is vital that the best practice is determined.
At our institution, it is common practice to obtain radiographs after hardware removal at the first follow-up appointment. The purpose of this study was to evaluate whether or not these post-operative radiographs alter treatment after uncomplicated removal of hardware. We hypothesized that routine post-operative radiographs do not change the expected course of patient care.
Following approval from our institutional review board, all removal of hardware procedures between January 1, 2008 and January 1, 2013 were identified from a prospectively collected trauma database using Current Procedural Terminology (CPT) code 20680, denoting removal of a deep implant. Each case was retrospectively evaluated for study inclusion by chart review. Patients undergoing lower extremity hardware removal due to pain attributable to the implant were eligible. Patients undergoing removal of hardware for any other reason were excluded. Specifically, patients undergoing hardware removal due to infection or due to the need for an additional procedure (i.e. nonunion) were excluded.
Demographic and injury information were recorded for all subjects meeting study criteria, including age, gender, initial injury and treatment, and date of hardware removal, and the number of radiographs obtained following hardware removal. Intra-operative fluoroscopy was available if needed for all procedures although the use of intra- or post-operative imaging was at the discretion of the treating surgeon.
Post-operative notes for these patients were reviewed to assess changes, if any, to clinical care following post-operative radiographs. A change was defined as any alteration in the expected post-operative course or treatment plan. These changes included, but were not limited to, additional intra-operative or post-operative imaging ordered, additional surgical intervention, changes in weight-bearing recommendations and/or changes in the intervals of follow-up appointments. Every patient was followed for a minimum of six weeks post-operatively. Additional short-term follow-up visits were not required due to the nature of the surgery, although patients were typically re-examined at one year from their index procedure.
All fees charged for foot and ankle radiographs were assessed and averaged, including radiology reading fees. The approximate charge for complete foot/ankle films, as reported by our institution’s radiology department, was determined. The estimated charge takes into account both the charge of the institution’s technical resources to take a full-length foot and/or ankle film series and also the professional services for interpreting the x-rays .
A total of 263 patients were investigated using the CPT code 20680. Of the 263 patients undergoing hardware removal between January 1, 2008 and January 1, 2013, 160 (60.8%) of them did not meet the inclusion criteria: 146 (91.3%) were excluded due to infection, non-union, or concurrent procedures (fusion or debridement) and 14 (8.7%) patients did not have a follow-up x-ray within the 60-day period following removal of hardware. 103 (39.2%) patients met the inclusion criteria (Figure 1) - 47 (45.6%) patients were male.. Patient age ranged from 15 to 70 years, with a median age of 43. Ankle fractures were the most common injury (44 patients, 42.7%), followed by pilon fractures (28 patients, 27.2%) (Table 1).
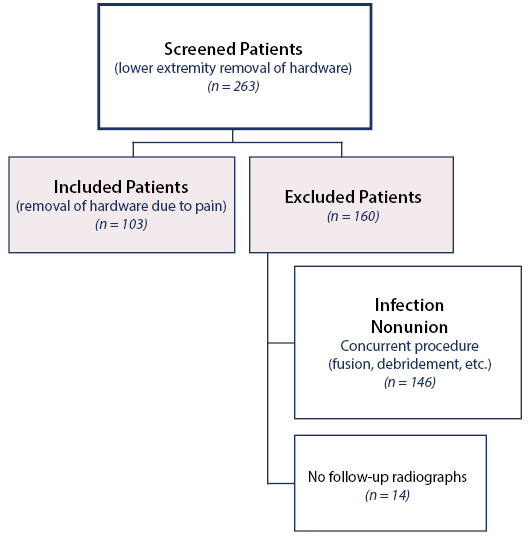
Demonstrates the number of patients included and excluded and the reasons for exclusion.
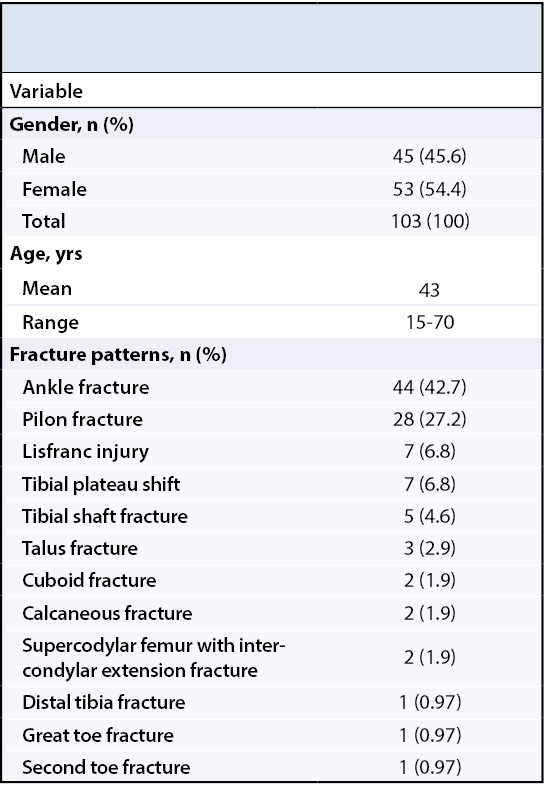
For all 103 patients (100%), the radiographs following hardware removal did not alter the pre-existing treatment plan, as assessed in the minimum 6-week follow up period.
The charge of a three-view ankle series was approximately $300, while the charge of a three-view foot series was approximately $315.
Radiographic imaging following orthopaedic procedures, especially removal of hardware from lower extremities, is a routine practice that has not been well-studied and is not supported by current evidence. Although post-operative radiographs allow the surgeon to assess bone alignment and healing in the absence of hardware, the value of this information remains to be elucidated for routine cases when the indication is simply pain.
Historically, medical legal factors have driven the common practice of obtaining post-operative radiographs. The radiopaque nature of bones and hardware allows for simple post-operative documentation in the form of radiographs. Consequently, it has become common practice to assess orthopaedic hardware removal in this manner. Perhaps the easy accessibility of obtaining radiographs, as opposed to legitimate clinical benefits, is what makes it such a common practice. Certainly, should complications occur after a surgery, a well-documented visual record of what was done is beneficial. If litigation ensues, a post-operative radiograph can elucidate the alignment of bones following hardware removal. Despite this potential benefit, the success of lower extremity hardware removal is primarily indicated by clinical assessment, unlike many other orthopaedic procedures where radiographic appearance is the main indication of the outcome. Thus, the value of these radiographs could be limited.
For our study cohort, which consisted of patients who had hardware removed from their lower extremity, we did not find a single case where a post-operative radiograph led to a change in clinical care for the patient. No musculoskeletal radiographic abnormalities other than the known healing/healed fractures were found in any of the 103 eligible patients, yielding no change to planned post-operative management. Thus, the data suggest that routine radiographs following hardware removal may be an unnecessary burden that should be limited to certain situations. Examples may include re-injury or presentation with pain that is out of proportion to expected levels for the postoperative course.
Our findings are consistent with others who have assessed the necessity of routine post-operative radiographs after various orthopaedic procedures. Miniaci-Coxhead et al. examined the utility and quality of formal post-operative radiographs following ankle fracture fixation and found that these radiographs did not contribute to patient care.12 Simpson et al. attained similar results when studying post-operative images following anterior lumbar interbody fusion.7 These same results have also been determined when post-operative radiographs were reviewed following supracondylar humerus fractures,13 hip fractures,8,9 osteotomies for hallux valgus,10 and shoulder arthroplasty.14
The rising cost of healthcare has prompted constant scrutiny towards management and efficiency. At our institution, the average charge for a three view ankle series is approximately $300 including the professional and technicial fees. The average charge for a three view foot series is approximately $315. Although these charges are not entirely representative of the collective cost of radiology due to the financial offset by insurance, the cost associated with unnecessary imaging is extraneous. Considering the high frequency of removal of hardware procedures,1 the cost savings from eliminating unnecessary postoperative radiographs could have a large financial impact.
There is also concern regarding exposure to ionizing radiation during radiographs. The FDA has strongly advised clinicians to order tests that will answer medical questions and/or modify patient care.15 Eliminating unnecessary radiographs may decrease exposure to ionizing radiation, which has been linked to cardiovascular disease5 and other health issues. That said, while appendicular radiographs do involve core radiation exposure, the risk is negligible (i.e. less than one in one million lifetime risk of an adverse event per radiograph) as described by Hendrick et al. These exams provide an estimated dose of 0.005 mSv with a calculated lifetime risk of cancer/lifetime adverse event at one in five million.16 Despite this negligible risk of an adverse event, it is nonetheless a concern to patients and should be considered by the ordering physician.
Previous studies have found an inverse correlation between office wait times and patient satisfaction.6 In order to reduce wait times and increase patient satisfaction, it is essential that maximum efficiency and throughput is attained. The current practice of obtaining radiographs following hardware removal is subjecting patients to unnecessary radiographs creating longer wait times. Thus, a more thoughtful approach in obtaining post-operative radiographs when clinically indicated will be a positive step towards reducing wait times and increasing efficiency.
The main limitation of this study is the retrospective methodology used. Though clinical and operative notes were recorded and analyzed, the only way to accurately assess changes in treatment plan would be to conduct the study prospectively. Furthermore, because the database utilized for the purposes of this study was an orthopaedic trauma database, all patients in this study had trauma-related injuries. Although we feel the results of this study are applicable to any patient with symptomatic hardware, they were not evaluated in this study. Furthermore, our cost analysis did not assess the costs offset by insurance, and was thus only an approximation of the cost associated with the foot/ankle radiographs.
In conclusion, routine post-operative radiographs after removal of hardware secondary to pain in a cohort of patients sustaining lower extremity trauma did not alter clinical course. By limiting the practice of obtaining these radiographs, practitioners can eliminate extraneous imaging, decrease radiation exposure, decrease costs, and save time.







