Hallux Valgus Surgery: A Technique to Assist with Soft-Tissue Correction
Michael S. Nirenberg, DPM
The author reports no conflict of interest related to this work.
©2022 by The Orthopaedic Journal at Harvard Medical School
Hallux valgus (HV) is one of the most common foot deformities, frequently involving soft-tissue contracture. A number of surgical methods have been used to release soft-tissue contractures associated with this progressive foot deformity. The impact of skin tightness as a component of soft-tissue contracture is unclear and has not been examined in peer-reviewed journals. To that end, a search of the literature failed to find any methods of soft-tissue release that addresses the skin.
The objective of this paper is to provide surgeons with a simple technique to assist in reducing soft-tissue contracture, including possible skin contracture, during HV surgery. This approach may lessen the need for more extensive bone procedures. The author has performed this technique on 10 patients, and it has been found to be safe, inexpensive, and easy to perform. Cautions and limitations of the technique are also described in this article.
LEVEL OF EVIDENCE Level V Expert Opinion
KEYWORDSHallux valgus; soft-tissue contracture; skin contracture; hallux valgus surgery; bunion surgery
Hallux valgus (HV) is a common foot deformity that occurs when the position of the great toe is angled at least 15° lateral to the first metatarsophalangeal joint (“first MTP”) toward the lesser toes.1 Hallux valgus often worsens gradually over time and can lead to arthritic and inflammatory sequela. This progressive foot deformity frequently results in the development of a painful prominence at the medial side of the first MTP, commonly known as a bunion. Hallux valgus may cause a callous or bursa to form at the prominence and can also contribute to general foot pain and impaired gait. In addition, HV may increase the risk for developing a pressure ulcer.5,22,43 A comprehensive review of literature found the prevalence of HV to be 23% for persons who are 18 to 65 years of age, and 35.7% for persons who are over 65 years old.25
Treatment for HV includes conservative measures, such as a change in footwear, taping, splinting, stretching/mobilization exercises, medication, injections, and soaks, along with the use of a spacer or toe separator, pads, and/or foot orthotics.2,15,17,45,47 Surgical measures for HV vary greatly and are often dependent on the severity of the deformity. Moreover, consideration often is given to other factors, such as the presence of concomitant bone or joint abnormalities (i.e. arthritis, osteopenia, or cystic changes), the nature and level of the patient’s pain, the patient’s circulatory status, and other comorbidities that may impact healing.12,17,32,36,37
Soft tissue contractures at the first MTP are thought to be a factor in the development of HV.27 Depending on the degree of HV deformity, most surgical procedures are frequently combined with release of the lateral soft tissues at the first MTP.3,13,31,46,49 The soft tissue release will typically involve transection of the distal attachment of the adductor hallucis muscle, the lateral metarsosesamoid suspensory ligament, and/or other ligaments associated with the fibular sesamoid bone and first MTP. More specifically, this entails the soft tissue release of the transverse metatarsal ligament to improve sesamoid realignment.8,13,31,35,49
Although satisfactory surgical results have been documented with HV procedures, complications have also been reported. Under-correction and recurrence are two of the more frequently seen complications.11,19,23,28 In addition, failure to realign the proximal phalanx over the first metatarsal head to establish a congruent joint has been linked to HV recurrence, surgical failure—and ultimately—patient dissatisfaction.23,28,36,44
In cases of moderate or severe HV deformity, defined as an HV angle of 20° to 40° or greater than 40°, respectively,9 reducing the lateral deviation of the hallux to create a congruous first MTP may be hindered. This is in part due to soft-tissue contracture.6,10,21,35,49 Once the surgeon has exhausted bone procedures and soft-tissue releases, there are limited options to address residual soft-tissue contracture, including any component of tension from the skin.
One approach has been the general recommendation to strap or splint the hallux after surgery for a period of time.16,24 The use of a Kirschner wire (K-wire) positioned down the length of the hallux, through the MTP, has been advocated in the Keller procedure for HV.29 Though, placing a K-wire through the MTP is not possible in some HV procedures, such as joint-replacement procedures or the use of some types of hardware.
These approaches may indirectly address tension from the skin, however, a search of the literature did not produce any articles that consider skin contracture as an independent deforming force on the hallux in HV surgery and thus, the skin’s influence in HV is unclear. As such, the effect of skin contracture—if present in HV—has not been addressed with soft-tissue release procedures.
The purpose of this article is to present a simple, safe technique that can be used during HV surgery to address soft-tissue contracture, including possible tension from the skin, to assist the surgeon in positioning the hallux in a rectus aligned position, congruent with the first metatarsal.
This technique is indicated during an HV procedure when the surgeon has exhausted bone and soft-tissue procedures and is unable to align the hallux congruent with the first metatarsal, such that soft-tissue “pulls” the hallux into a lateral-proximal position (i.e., tilted toward the second toe). Typically, this has been observed in long-standing, severe HV deformity, although it could be present in lesser HV deformities.
To address this, the surgeon must grasp the hallux with two fingers and position it in a rectus position. He or she must then gently pull the toe distally, exerting slight tension on the soft-tissues. This distal position of the hallux allows the first MTP to “open” or distract, forming a joint space. A K-wire is then inserted into the distal-medial aspect of the hallux’s proximal phalanx. The wire is inserted in a proximal direction into the second metatarsal head. The recommended K-wire size is a 0.062 of an inch (1.6mm); however, if the patient’s bone stock is poor, a 0.045 of an inch (1.1mm) size can be used to reduce the risk of fracture. The entry point of the K-wire should be midway between the dorsal and plantar aspect of the hallux to avoid injury to the sensory nerves, which course in these areas. Based on the surgeon’s preference, fluoroscopy can be used (Figures 1-3). After the K-wire is positioned, the protruding end is bent to 90° and covered with a protective cap.
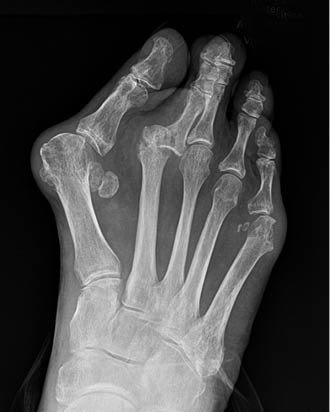
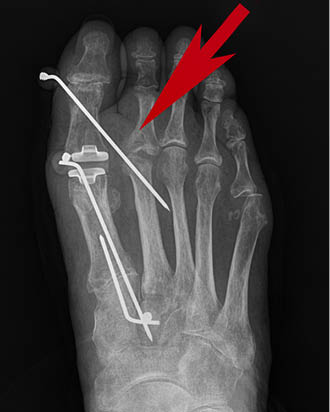
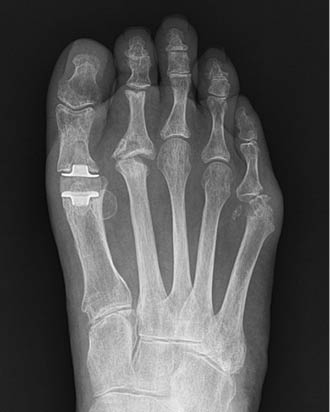
To protect the foot, the patient is prescribed a hard, flat-soled surgical shoe or walking boot. This prevents the foot from bending. The K-wire will remain in the foot for six to eight weeks; however, in some cases, the wire will loosen, requiring an earlier removal. The described technique has been used with 10 patients without any untoward effects. Patients were monitored for a minimum of four months with eight of the subjects maintaining a satisfactory result, which is defined as a HV angle less than 15°.9 Two patients experienced a recurrence of HV. These HV deformities were less severe than prior to surgery and were asymptomatic. The patients still found their results to be satisfactory.
The goal of this technique is to achieve normal anatomic alignment of the hallux in HV surgery, and this technique may further the restoration of the first MTP’s congruity for some patients, and as a result, could lessen the chance of HV recurrence.11,28,32
Alternatives to the clinical suggestion presented in this article include a procedure to fuse the first MTP,7 or to utilize strapping or splinting methods.16,24 Depending on the degree of HV deformity, however, these methods may not adequately counteract the soft-tissue pull on the hallux. Also, patient movement is more likely to displace a splint or strapping than it is to dislodge a K-wire.
From anecdotal observation, part of the soft-tissue contracture in some of the more severe HV deformities involves the skin. The ability to stretch skin and its associated soft-tissues over time, the use of devices and techniques to close skin defects or ulcers, as well as reduce contractures are well-established.4,14,18,26,30,38,39,42 K-wires have been utilized by surgeons in a number of ways to assist with the stretching of skin (and the underlying soft-tissue).34,48
The success of K-wires and these other devices is a result of the skin’s viscoelastic properties that allow it to stretch beyond its physiological limit when subjected to continuous force.30,40,41 This force activates two phenomena: mechanical and biologic creep. The former relatively quickly causes the morphology of cells to stretch; while the later, biologic creep, occurs over many weeks and involves cellular proliferation, increasing surface area.20,33 The effects of the process maximize at 6 to 12 weeks, wherein the epidermis thickens and the dermis thins.20
During HV surgery, the possible need of this technique to address residual soft-tissue with possible skin contracture is determined intraoperatively after the bone procedure(s) and release of the soft tissues has been performed. This technique appears most advantageous in severe HV deformity of long duration. In such cases, multiple concomitant procedures may be required to correct related foot issues. That was true of the case depicted in the radiographs shown herein. In the presented case, the K-wire enters the head area of the second metatarsal; however, the procedure has also been successful with placing the K-wire in the distal shaft of the second metatarsal. It should be noted that a possible consequence of placing the K-wire in the shaft is an increased risk of metatarsal fracture.
The indication for this technique is the need to address residual soft-tissue contractures, including any tension from the skin, limiting a congruous first MTP in HV surgery. But relative contraindications include peripheral vascular disease or poor soft-tissue or skin integrity. In most scenarios, patients with such issues would not be surgical candidates. For those exceptions, however, surgeons should be cognizant that placing tension on soft-tissues and/or skin can exert similar force on the underlying subcutaneous tissue and blood vessels. As a result, viability could be compromised in some patients, particularly if excessive force is applied, or the soft-tissue or skin integrity is impaired. Therefore, the soft-tissue and skin around the first MTP should be evaluated prior to performing this technique. If they appear unhealthy, discolored, or atrophic, the surgeon must proceed with caution or abandon the use of this technique.
A possible complication of this technique is the K-wire bending or even breaking. To lessen this risk, besides having patients wear a hard, flat post-operative shoe, they should also be instructed to walk flat-footed and avoid bending their toes.
In the 10 patients who required this technique, it is uncertain why two of them saw the HV deformity recur. The literature shows that recurrence in HV surgery is among the most common complications with a variety of possible causes.11,19,23,28 Clearly, more research into this technique and perhaps modifications to it is warranted. Such investigation should include a longer follow-up and greater number of patients. In addition, these studies should consider the effect of maintaining the hallux in its rectus position for a longer duration after surgery.
Hallux valgus surgery can be challenging, and in some cases, long-standing soft-tissue contractures of the first MTP can negatively impact outcomes. This paper presents a safe, simple, and inexpensive technique of using a K-wire to address contractures of the soft-tissues, including possibly lessening skin tension, in HV surgery. This article is aimed at stimulating further investigation into the effect of soft-tissue contracture and initiating additional research into skin tension in HV deformity and surgical correction.
In sum, this technique may improve alignment of the hallux during HV surgery and ultimately, provide the patient with a better result.






