Concise Review on Surgical Fixation of Distal Humerus Fractures
Grace Xiong, MD and Abhiram R. Bhashyam, MD, PhD
The authors report no conflict of interest related to this work.
©2020 by The Orthopaedic Journal at Harvard Medical School
Distal humerus fractures are an increasingly common injury with complex anatomy which can be challenging to treat. The primary goal of treatment is to recreate a mobile, painless, stable joint. In this review, we address anatomic considerations, fracture classification systems, as well as options for exposure, fixation principles, and available implants.
LEVEL OF EVIDENCE Level V Review
KEYWORDS Distal humerus fractures, trauma, geriatric trauma
Distal humerus fractures are becoming increasingly common, especially among older male patients.1,2 These injuries are challenging to manage, often adversely affecting patient independence and with poor outcomes. As with many fractures, distal humerus fractures have a bimodal distribution-typically affecting younger patients via high energy mechanisms and older patients via low energy trauma or falls.3 In the elderly population, distal humerus fractures often portend a decline in independence in activities of daily living from which it can be difficult to recover.4 The primary goal of treatment is to recreate a stable, mobile, painless joint.5-7 Ideally, these aims are achieved in a durable manner that diminishes the risk of post-traumatic arthritis and reoperation.
The anatomy of the elbow joint contributes to challenges in the management of distal humerus fractures. The distal humerus is composed of a medial and lateral column connected at the articular surface by a “tie arch,” similar to arched bridges supported by the underlying bridge deck rather than the ground. This keystone, which connects the medial and lateral columns, is what gives the distal humerus its intrinsic stability, even in osteoporotic bone. The trochlea and capitellar articular surfaces project approximately 40 degrees anterior to the anatomic axis of the humerus. When viewed in the coronal plane, the “tie arch” also sits in a position approximately 4-8 degrees valgus compared to the mechanical axis which allows the physiologic carrying angle to carry objects away from the body.8,9
Due to the complexity of distal humerus anatomy, several classifications have been developed to describe these potentially complex fractures.10 The AO/OTA classification is commonly used and, following standard AO nomenclature for all fractures, and encompasses several components.5 The first component, “1”, refers to the humerus in standard AO referencing with “3” indicates the distal segment, followed by letter designation according to degree of articular involvement. “A” fractures are entirely extraarticular, type B fractures are partial articular fractures with some portion of the humerus still intact with the articular surface, and type C fractures are intraarticular fractures with no preserved diaphyseal-epiphyseal connection. Further fracture sub-types are based on specific patterns and degree of comminution.
Other classifications include the Milch11 and Jupiter9 systems. The Milch system is designated based on if the lateral trochlea is still attached to the humeral shaft. In type I fractures, the lateral eminence of the trochlea remains attached and the fracture line passes medial, whereas type II fractures involve the trochlear ridge and articular surface. The Milch system is useful for interpreting distal humerus fractures, however was more important before the advent of locked plating and is primarily used for research purposes in the current clinical environment. The Jupiter classification is based off the concept of a mechanical triangle, with the medial column, lateral column, and trochlea comprising the sides of the triangle or “arch”. The classification is divided into intraarticular, extraarticular intracapsular, and extracapsular fractures. Intraarticular fractures are further divided into single- and bi-columnar fractures, capitellar fractures, and trochlear fractures.
In general, operative management is indicated for most distal humerus fractures to optimize functional outcomes and achieve a stable, mobile, painless joint. The standard operative treatment is open reduction and internal fixation with either unicolumnar or bicolumnar plating. Exceptions to this treatment approach include geriatric, low-demand patients who are unable to tolerate or participate in postoperative rehabilitation protocols,12,13 as well as medically unwell patients for whom the risk of surgery would outweigh benefits. For these patients, some have advocated a conservative management strategy (“bag of bones”), in highly comminuted fractures in low demand patients, while others have recommended total elbow arthroplasty for highly comminuted fractures for patients who still retain enough functional demand that the “bag of bones” technique does not afford adequate function.12,14,15 It is imperative that appropriate counseling be undertaken to inform the patient of risks of non-operative management such as the decrement in range of motion.
In addition to standard radiographs of the elbow (anteroposterior and lateral views), two additional imaging techniques can significantly aid in pre-operative planning. A traction radiograph can help to define articular fragments and aid in pre-operative classification of the fracture. In addition, recent studies have demonstrated that computed tomography, especially with three-dimensional reconstruction, can help improve identification of single fragments, articular surfaces and fracture edges. This additional information has been shown to be especially useful for pre-operative planning of fracture reduction and implant selection.7,8,16,17 CT is particularly useful for identifying impacted fracture fragments that make reduction challenging.
Strategy for surgical fixation
Operative management of distal humerus fractures should prioritize stable fixation. Given the multi-directional physiologic forces on the elbow joint during functional activity, stable fixation devices are necessary to avoid subsequent implant failure. A typical tactic based on AO principles for reconstruction of the distal humerus is:
- Anatomic articular reduction with stable internal fixation
- Restoration of articular axial alignment with stable internal fixation of the articular segment to the metaphysis and diaphysis
- Early range of motion
For fracture patterns with large supracondylar or cartilage defects, additional treatment principles involve:
- Judicious use of provisional internal fixation to restore the articular block
- Bone graft (allograft or autograft) to fill any bony meta-diaphyseal bony defects
In this review, we do not cover total elbow arthroplasty for management of comminuted distal humerus fractures in older-age, low-demand patients or those with severely osteoporotic bone as this has been covered in other recent publications.14,15
Strategy for surgical fixation
The three most common posterior approaches used for exposure of distal humerus fractures are the triceps split, paratricipital, and the olecranon osteotomy. The primary considerations in selection of one of these approaches is the amount of exposed articular surface that can be visualized or preservation of alternate surgical strategies (e.g. keeping the option for total elbow arthroplasty if appropriate reduction and stable fixation cannot be obtained in elderly patients). Anatomical studies have demonstrated that the median exposed articular surface for the paratricipital, triceps splitting and olecranon osteotomy approaches are 26%, 35-37%, and 52-57% respectively.18,19 Despite wide exposure, achieving an anatomical reduction of the articular surface in a highly comminuted fracture can be challenging.
Another more recent approach that has been described is the triceps-reflecting aconeus pedicle (TRAP) approach.20 In this approach, the triceps is reflected off of its olecranon attachment and the anconeus off its ulnar attachments via a longitudinal posterior approach. The triceps and the anconeus pedicle are then retracted proximally, allowing full visualization of the joint once the elbow is placed in full flexion. This approach provides similar exposure as that of an olecranon osteotomy, save for a portion of the anterior trochlea. Proponents of the technique cite the use of the existing olecranon, coronoid, and radial head as anatomic templates which can aid in the reduction of distal humerus fragments.
O'Driscoll principles and technique
In the management of intra-articular distal humerus fracture fractures, O’Driscoll proposed two principles to guide operative planning for distal humerus fractures:8
- Maximize fixation in the distal fragments
- All fixation in the distal fragments should contribute to stability between the shaft and the distal fragments
He went on to propose eight technical details, which we condense and summarize here:
- Every screw in the distal fragment should pass through a plate from the opposite column to maximize distal fixation as well as fixation to the shaft.
- Every screw in the distal fragment should engage as many articular fragments as possible
- The screws in distal fragments from the medial and lateral columns should interdigitate, indirectly providing a fixed angle device with as many screws (of maximum possible length) as possible. This reconstitutes what O’Driscoll termed a “keystone” concept, also referred to as the trochlea in “tie arch” concept.
- The plates should be applied with compression at the supracondylar level and be strong enough and stiff enough to resist failure until union occurs
Parallel versus orthogonal plating
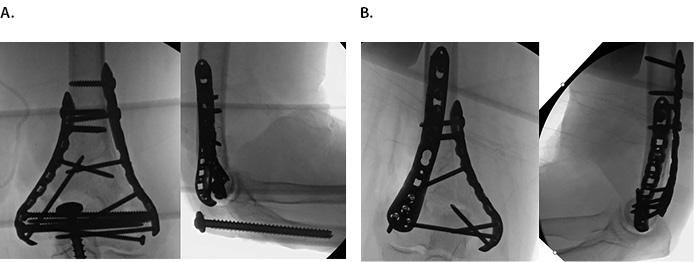
Multiple studies have compared clinical and biomechanical results of parallel plating versus orthogonal plating for distal humerus fixation (parallel: Figure 1A, orthogonal: Figure 1B). A recent meta-analysis of seventeen biomechanical studies demonstrated greater strength and stiffness in axial (difference 225.0 N/mm) and torsional loads (difference 0.58 Nm/deg) in parallel plating compared with orthogonal plating.22 In clinical practice, a recent systematic review and meta-analysis of 6 RCTs and 2 cohort studies demonstrated no difference between groups in postoperative range of motion, however this analysis did note a decreased time to union in parallel plating versus the orthogonal plating group (standard mean difference 0.36 although absolute times not reported, P = 0.018).23 Based on these reports, the decision to use parallel versus orthogonal plating strategies should remain at the discretion of the surgeon based on the fracture type.
Implant options
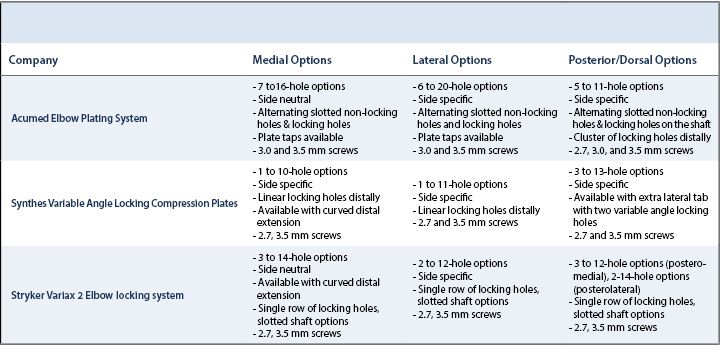
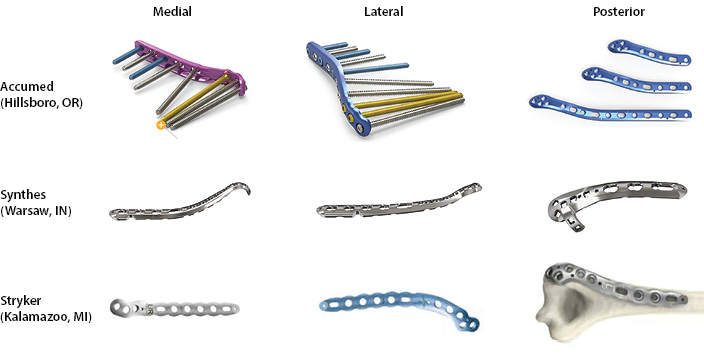
To address the specific needs of distal humerus fractures, several implants are available. Most companies offer some combination of medial, lateral, and dorsal-specific plating with locking options. Locking options may be favored, particularly in osteoporotic bone to aid in resistance to torsional loads.24,25 These options are summarized in Table 1 by company with example images in Figure 2.
In summary, distal humerus fractures are an increasingly common injury that has significant implications for patient’s functional independence in activities of daily living. Surgical fixation of these injuries is the most common treatment option, with conservative “bag of bones” or total elbow arthroplasty techniques reserved for older-age, lower-demand patients. Multiple treatment strategies and implant options exist for management of distal humerus fractures based on fracture and patient characteristics. To achieve the best outcome possible an anatomic reduction of the joint surface needs to be achieved and stabilized with implants that allow for early motion and rehabilitation. Consideration of patient functional demand, fracture morphology, and available approaches are important for achieving an optimal long-term outcome.